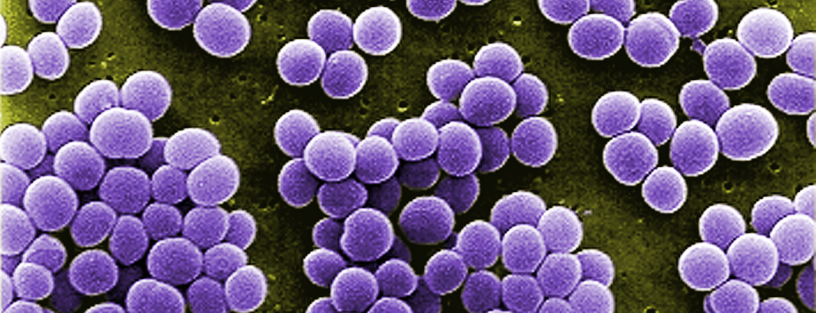
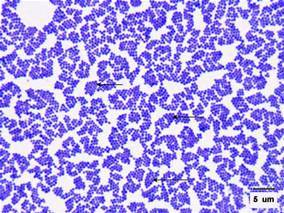
What do you know about Staphylococcus aureus? It’s one of the most common causes of foodborne disease, but is not the most commonly reported, why? This Gram positive coccus (Figure 1) generally results in a relatively mild and self-limiting disease with fatalities extremely rare. However, it still sickens many and impacts on the economy due to absences from work and occasional hospitalisations. Let’s find out more about this pathogen…
What are their preferred growth conditions?
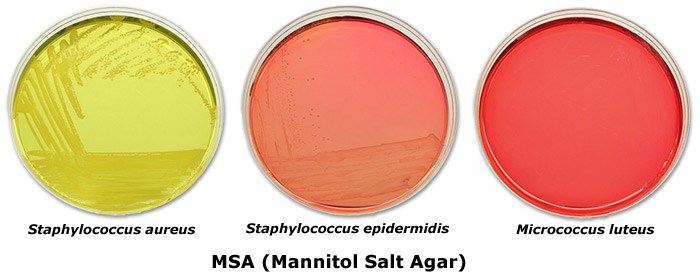
The optimal growth conditions for S. aureus are as follows: Temperature between 30 °C and 37 °C, water activity between 0.94 and 0.99, pH slightly alkaline in the range of 7.0 to 7.5, and an aerobic atmosphere. They are also very salt tolerant, even more so Vibrio spp. which thrive in the seas and oceans of the world. S. aureus can tolerate an NaCl concentration as high as 15%, and in fact this is exploited in its isolation, for example with Mannitol Salt Agar (MSA) (Figure 2). MSA is a selective medium for staphylococci due to the incorporation of 7.5% NaCl, which ensures almost nothing else is capable of growing. Due to its salt tolerance, S. aureus is not an uncommon human skin commensal, which contributes to the ease of its transfer onto food, from food handlers. Not infected food handlers, because various species of staphylococci can be found in/on various human body locations as a normal part of the microbiome.
What is the pathogenesis of staphylococcal intoxication?
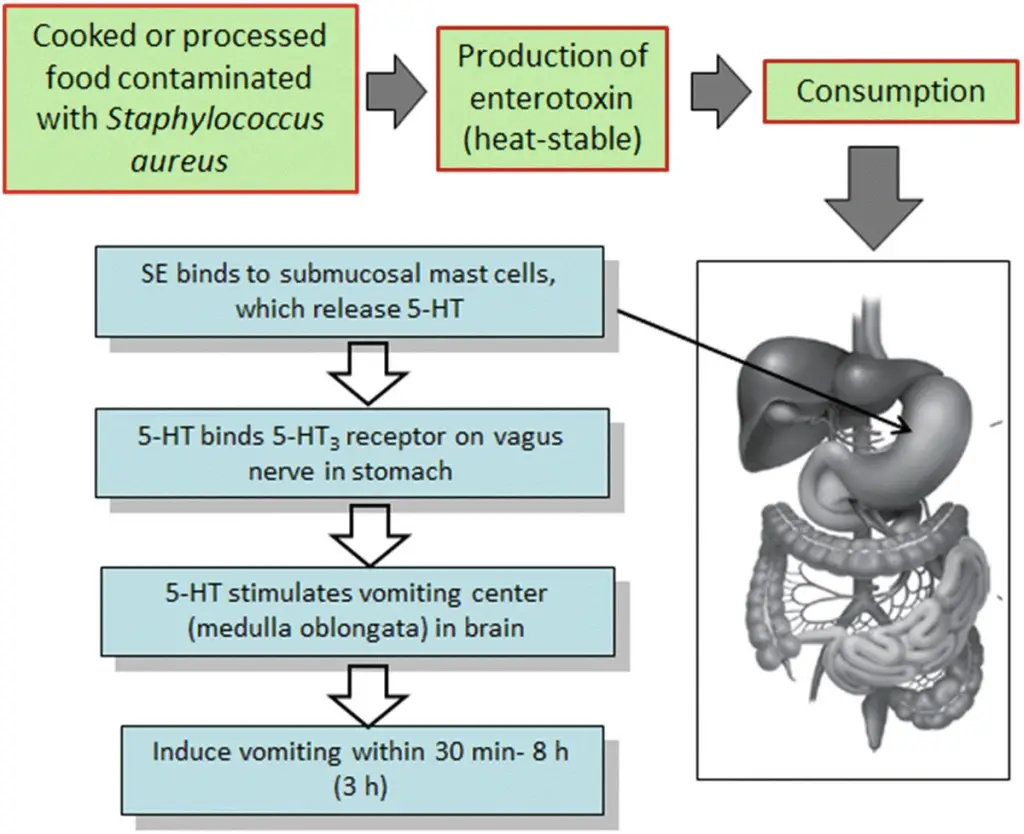
S. aureus produces enterotoxins. Their toxins (plus some produced by Streptococcus pyogenes) are collectively termed pyogenic toxins and act as super antigens. Unless a substantial dose of the toxin is ingested, their sit of action is localised in the abdominal viscera. In the abdomen, the toxin stimulates neural receptions, which then transmits impulses to the medullary emetic centre via the vagus and sympathetic nerves (Figure 3). Once the emetic centre is stimulated, vomiting results.
What is the clinical presentation of staphylococcal intoxication?
A patient diagnosed with staphylococcal foodborne disease usually presents with nausea, vomiting, diarrhoea and abdominal cramps which vary insecurity. While the symptoms are not long-lasting, with recovery typically taking place between 24 and 72 hours after the onset of symptoms, onset is rapid, since this disease is an intoxication. Symptoms are often seen around six hours after ingestion of the offending food item.
Mode of transmission
S. aureus is commonly found on human skin, such as hands. Since so many people carry this microorganism on their hands, this is one of the most likely ways for an outbreak to start. Nasal carriage is also common. In fact, nasal carriage is so common that analysing nasal carriage rates amongst university students is a favourite introductory activity in introductory microbiology laboratory classes. So, a typical example of transmission could run like this: A food handler carrying this bacterium is preparing food with barehands. The bacteria are transferred to the food during the preparation of the food for cooking. During this stage, when the bacteria are in the food, they grow and produce enterotoxins if the food is subjected to temperature abuse which would give the bacteria sufficient time to grow. The food is then cooked, which eliminates the bacteria, bu t not the extremely heat-resistant toxin, which can retained activity following standard cooking procedures. Believing the food to be safe for consumption after a normal cooking time and temperature, then food is served and consumed. Since the toxin remains in the food, intoxication results once the food is consumed, with onset symptoms typically seen in around six hours. Milk, cream sweets/cakes (Figure 4) and salty foods like ham are most often implicated.
What toxins are produced by S. aureus?
This species produces nine enterotoxins, designated A, B (Figure 5), C1, C2, C3, D, E, G and H. It would appear that enterotoxin A is probably respondislb for most staphylococcal intoxications. This has been the finding in a number of studies which isolated toxins from isolates which had been implicated in outbreaks of staphylococcal foodborne disease.
There are some staphylococcal outbreaks from high acid/low pH foods. How is this possible? Doesn’t the harsh acidic conditions eliminate the vegetative cells?
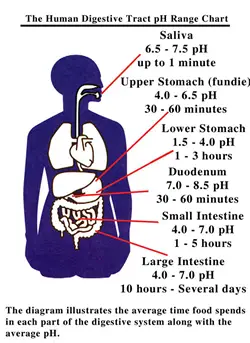
S. aureus is one of various bacterial species that are able to induce an acid tolerant state. This means that when the cells are subjected to a sub-lethal pH value, for example 5.0, they can adapt to acidic conditions sufficiently so that they can then survive at a much lower pH value, say 3.0, which would normally prove lethal. This has major implications for the food industry and for public health – take this example: A particular food that has a pH of around 5.0 is contaminated with cells of S. aureus. After exposure to this pH, and it doesn’t take long, maybe 15 or 30 minutes is all it takes, the cells become adapted to acidic conditions. The cells may not grow, but will remain viable in this pH 5.0 food. Then, when someone consumes the food (and the S. aureus cells), it is ingested and passes through the gastrointestinal tract (Figure 6). Once reaching the stomach, the pH of which is normally a lethal barrier to invading pathogenic microorganisms, the cells are able to survive and may result in disease at some point along the gastrointestinal tract. Even if they don’t, they could be shed in faeces as viable cells. This adaptation, for S. aureus, can take place in either inorganic or organic acid, which makes this circumstance of particular concern for the food manufacturing industry.